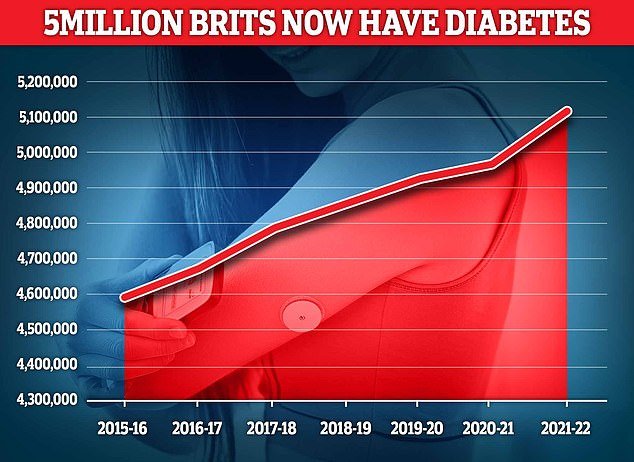
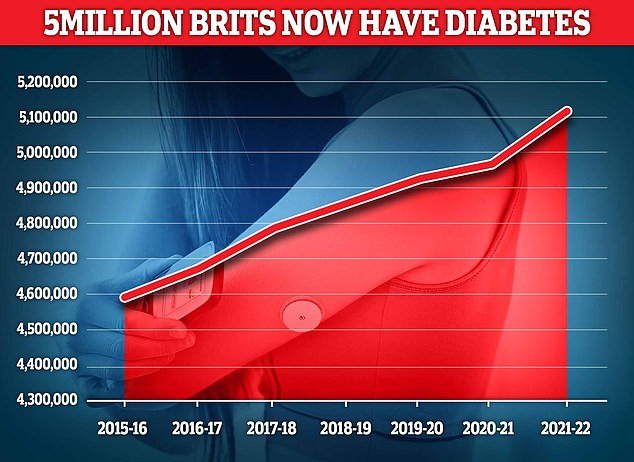
Depression has emerged as a significant and often overlooked factor in the development of type 2 diabetes. Emerging research has shed light on the strong interconnection between these two conditions, with individuals diagnosed with diabetes having a twofold increased risk of experiencing depression. Recent studies have further identified seven genetic variants that are implicated in both conditions, offering a novel perspective on the shared biological mechanisms underlying their association. Recognizing the reciprocal relationship between depression and type 2 diabetes, health officials are now urged to view depression as an independent risk factor for the development of the metabolic disorder. Furthermore, efforts should be made to address and prevent the onset of type 2 diabetes at the early stages of depressive symptoms, considering the substantial impact that living with diabetes can have on an individual’s mental health.

The Link Between Depression and Type 2 Diabetes
Depression and Type 2 diabetes are two prevalent and complex health conditions that often coexist, with evidence suggesting a bidirectional relationship between the two. It is important for healthcare professionals to understand this link and its implications to provide optimal care for individuals dealing with both conditions.
Depression as a Risk Factor for Type 2 Diabetes
Depression has been identified as a risk factor for the development of Type 2 diabetes. Research has shown that individuals with depression are more likely to develop diabetes compared to those without depression. This association holds true even after accounting for other risk factors such as obesity and physical inactivity.
A study conducted by Dr. Edwin W. Williams and his colleagues at Harvard University examined the relationship between depression and diabetes. The study found that depressed individuals have a 37% increased risk of developing Type 2 diabetes compared to those without depression. This suggests that depression can play a direct role in the development of diabetes.
Higher Prevalence of Depression in People with Diabetes
On the other hand, individuals with diabetes have a higher prevalence of depression compared to the general population. Studies have consistently shown that people with diabetes are twice as likely to suffer from depression as those without diabetes. This increased risk may be attributed to the challenges associated with managing a chronic illness and the psychological impact of living with diabetes.
The burden of living with diabetes, such as the need for self-care, strict dietary restrictions, and regular monitoring, can contribute to the development of depression. The constant management of blood sugar levels and the fear of complications can lead to feelings of distress and overwhelm. Therefore, healthcare professionals should consider depression as a risk factor when caring for individuals with diabetes.
Genetic Variants Contributing to Both Depression and Type 2 Diabetes
Recent advancements in genetic research have revealed that there are common genetic variants that contribute to both depression and Type 2 diabetes. A study conducted by Dr. David J. Cutler and his team at the Massachusetts General Hospital and Harvard Medical School identified seven genetic variants that are associated with both conditions.
These findings suggest a shared genetic vulnerability and provide further evidence for the link between depression and Type 2 diabetes. Understanding the genetic underpinnings of both conditions can help in developing targeted interventions and personalized treatment approaches.
Understanding the Relationship
To fully comprehend the link between depression and Type 2 diabetes, it is crucial to explore the various mechanisms and factors influencing this relationship. Several factors contribute to the development of both conditions, including shared biological pathways, chronic stress, inflammation, insulin resistance, and medication side effects.
Shared Biological Pathways
Depression and Type 2 diabetes share several biological pathways, implicating common underlying mechanisms. For instance, dysregulation of the hypothalamic-pituitary-adrenal (HPA) axis, which is involved in the stress response, has been observed in both depression and diabetes. This dysregulation may contribute to the development of insulin resistance and impair glucose metabolism.
Additionally, abnormalities in neurotransmitters such as serotonin, dopamine, and norepinephrine, which are implicated in mood regulation, have been associated with both conditions. These shared biological pathways highlight the intricate interplay between depression and Type 2 diabetes.
Impact of Chronic Stress
Chronic stress is a common factor in both depression and Type 2 diabetes. Stress activates the HPA axis, leading to increased levels of cortisol, a stress hormone. Prolonged exposure to high levels of cortisol can contribute to insulin resistance and disrupt glucose regulation, ultimately increasing the risk of developing diabetes.
Moreover, chronic stress can also affect mental health, leading to the development of depression. The constant strain and pressure associated with managing diabetes can be psychologically distressing, further exacerbating the risk of depression.
Inflammation and Insulin Resistance
Inflammation and insulin resistance play crucial roles in the development of both depression and Type 2 diabetes. Inflammation disrupts insulin signaling pathways, leading to insulin resistance, a hallmark of Type 2 diabetes. It also affects the brain’s neurotransmitter balance, contributing to the development of depressive symptoms.
Furthermore, chronic inflammation, a characteristic feature of Type 2 diabetes, has been linked to the pathophysiology of depression. The presence of inflammatory markers, such as C-reactive protein (CRP) and interleukin-6 (IL-6), has been associated with an increased risk of depression. Understanding the interaction between inflammation and insulin resistance can provide insight into the shared etiology of depression and Type 2 diabetes.
Medication Side Effects
Certain medications used in the treatment of depression and diabetes can also contribute to the development or exacerbation of the other condition. Some antidepressant medications, such as selective serotonin reuptake inhibitors (SSRIs), have been associated with weight gain, metabolic disturbances, and an increased risk of developing diabetes.
Similarly, some medications used to manage diabetes, such as corticosteroids, can have mood-altering effects and contribute to the development of depressive symptoms. Healthcare professionals should be aware of these medication side effects and carefully consider their use when treating individuals with comorbid depression and Type 2 diabetes.
Depression as a Risk Factor
Depressive symptoms can have a significant impact on health behaviors, contributing to an increased risk of developing Type 2 diabetes. Understanding these associations can help identify individuals at risk and implement preventive strategies.
Depressive Symptoms and Health Behavior
Depression is often associated with unhealthy lifestyle choices, including poor dietary habits, physical inactivity, smoking, and excessive alcohol consumption. These behaviors, collectively known as “depressive health behaviors,” increase the risk of developing obesity, insulin resistance, and subsequently, Type 2 diabetes.
Individuals with depression may experience a lack of motivation, energy, and interest in engaging in physical activity or adhering to a healthy diet. Addressing these depressive symptoms through appropriate interventions and support can help mitigate the risk of developing Type 2 diabetes.
Altered Sleep Patterns
Sleep disturbances are commonly experienced by individuals with depression and have been linked to an increased risk of developing Type 2 diabetes. Depressive symptoms, such as insomnia and hypersomnia, can disrupt normal sleep patterns, leading to metabolic dysregulation and insulin resistance.
Research has shown that individuals with shorter sleep durations and those with poor sleep quality are at a higher risk of developing diabetes. Healthcare professionals should inquire about sleep disturbances when assessing individuals with depression and consider interventions to improve sleep hygiene.
Weight Gain and Sedentary Lifestyle
Weight gain and a sedentary lifestyle are common outcomes of both depression and Type 2 diabetes. Depressive symptoms can lead to emotional eating, resulting in weight gain and an increased risk of obesity. This weight gain, in turn, contributes to the development of insulin resistance and diabetes.
Furthermore, depression often leads to a decrease in physical activity and motivation to engage in exercise. Sedentary behavior is associated with an increased risk of developing Type 2 diabetes, independent of weight status. Encouraging regular physical activity and implementing lifestyle modifications can help prevent the onset of diabetes in individuals with depressive symptoms.
Poor Glycemic Control
Depression can also adversely affect glycemic control in individuals with diabetes. The burden of managing both conditions concurrently can be overwhelming and lead to decreased adherence to diabetes self-care behaviors, such as medication adherence, glucose monitoring, and healthy eating.
Moreover, depressive symptoms can affect an individual’s ability to cope with stress, further impacting glycemic control. Poor glycemic control increases the risk of diabetes-related complications and adversely affects overall health outcomes. Identifying and addressing depressive symptoms early on can help improve glycemic control and prevent long-term complications.
Prevention and Early Intervention
Recognizing the bidirectional relationship between depression and Type 2 diabetes is crucial for implementing effective prevention and early intervention strategies. Identifying individuals at risk, promoting physical activity and healthy lifestyle choices, and supporting emotional well-being can significantly reduce the burden of both conditions.
Identifying Depression in Individuals at Risk for Type 2 Diabetes
Healthcare professionals should screen individuals with prediabetes or those at high risk of developing Type 2 diabetes for depressive symptoms. Early identification of depression can lead to timely intervention and preventive strategies targeting both conditions.
Questionnaires such as the Patient Health Questionnaire-9 (PHQ-9) or the Beck Depression Inventory (BDI) can be used to assess depressive symptoms. A comprehensive evaluation of mental health should be incorporated into routine diabetes care to identify individuals who may benefit from additional support.
Integrated Approach to Treatment and Management
An integrated approach to treatment and management is essential in addressing the complex needs of individuals with comorbid depression and Type 2 diabetes. Collaborative care models, involving a multidisciplinary team of healthcare professionals, can optimize outcomes by providing coordinated and holistic care.
This approach typically involves close collaboration between primary care providers, mental health professionals, and diabetes specialists. By addressing both physical and mental health needs, integrated care models can improve treatment adherence, glycemic control, and psychological well-being.
Promoting Physical Activity and Healthy Lifestyle Choices
Prevention efforts should focus on promoting physical activity and healthy lifestyle choices in individuals with depression. Engaging in regular exercise has been shown to have positive effects on mood, reduce depressive symptoms, and improve glycemic control.
Healthcare professionals should encourage patients to incorporate physical activity into their daily routine and provide resources and support to help them overcome barriers to exercise. Additionally, promoting a healthy diet and weight management can further reduce the risk of developing or exacerbating both conditions.
Supporting Emotional Well-being
Supporting emotional well-being is crucial in individuals with comorbid depression and Type 2 diabetes. Psychoeducation, counseling, and support groups can provide individuals with the necessary tools and coping strategies to manage both conditions effectively.
Healthcare professionals should allocate sufficient time and resources to address the psychological needs of individuals with comorbid depression and diabetes. Providing access to mental health professionals, educating patients about the bidirectional relationship between depression and diabetes, and promoting self-care and stress management techniques can contribute to better overall health outcomes.
Implications for Healthcare Professionals
Understanding the implications of the link between depression and Type 2 diabetes is essential for healthcare professionals to provide comprehensive care. Screening for depression in diabetes care, implementing collaborative care models, offering educational programs, and providing mental health training are key considerations for optimizing patient care.
Screening for Depression in Diabetes Care
Screening for depression should be an integral part of diabetes care. Routine assessment of mental health can help identify individuals at risk and facilitate early intervention. Screening tools such as the PHQ-9 or BDI can be used to assess depressive symptoms and guide appropriate referrals and treatment.
Healthcare professionals should be attentive to changes in mood, appetite, sleep patterns, and motivation in individuals with diabetes. By actively addressing depression, healthcare providers can improve mental health outcomes, enhance treatment adherence, and reduce the risk of developing complications.
Collaborative Care Models
Collaborative care models, involving a multidisciplinary team, offer an effective approach to managing individuals with both depression and Type 2 diabetes. By integrating mental and physical healthcare, these models ensure that individuals receive comprehensive and coordinated care.
A collaborative care team typically consists of primary care providers, mental health professionals, diabetes specialists, and other relevant healthcare professionals. Regular communication and shared decision-making among team members facilitate the implementation of evidence-based interventions and promote optimal outcomes for patients.
Educational Programs for Patients
Educational programs play a vital role in empowering patients to manage both depression and diabetes effectively. Providing information about the bidirectional relationship between the two conditions, as well as self-care strategies, can empower individuals to take control of their health.
These programs should focus on educating patients about the importance of physical activity, healthy eating, medication adherence, stress management, and seeking appropriate support. By equipping individuals with the knowledge and skills to self-manage both conditions, healthcare professionals can improve overall health outcomes and quality of life.
Providing Mental Health Training
Healthcare professionals should receive adequate training in identifying and managing mental health issues in individuals with Type 2 diabetes. This training can help providers recognize the signs and symptoms of depression, screen for mental health concerns, and initiate appropriate interventions.
By enhancing mental health literacy among healthcare professionals, individuals with comorbid depression and Type 2 diabetes can receive timely and effective care. Training programs should incorporate evidence-based practices for depression management, self-care support, and strategies for promoting emotional well-being.
Psychological Impact of Living with Type 2 Diabetes
Living with Type 2 diabetes can have a significant psychological impact on individuals, contributing to the development of depression. The challenges associated with managing diabetes, the emotional toll of the diagnosis, and the impact on overall quality of life should not be overlooked.
Increased Risk of Developing Depression
The burden of managing a chronic illness like Type 2 diabetes can significantly increase the risk of developing depression. The constant need for self-care, adherence to a strict dietary regimen, regular blood sugar monitoring, and the fear of complications can lead to feelings of distress, sadness, and hopelessness.
It is crucial for healthcare professionals to be vigilant in identifying and addressing depressive symptoms in individuals with Type 2 diabetes. By providing the necessary support and interventions, healthcare providers can improve mental health outcomes and positively impact overall well-being.
Challenges in Diabetes Self-Care
Living with Type 2 diabetes often involves complex self-care regimens. Individuals must monitor their blood sugar levels, adhere to medication schedules, engage in regular physical activity, and follow a healthy diet. These demands can be physically and emotionally draining, posing significant challenges for individuals with depression.
Depressive symptoms, such as lack of motivation, fatigue, and difficulty concentrating, can interfere with diabetes self-care practices. This can result in suboptimal glycemic control, increased risk of complications, and a decreased quality of life. Healthcare professionals should provide tailored support and education to help individuals overcome these challenges and effectively manage both conditions.
Impact on Quality of Life
Type 2 diabetes can have a profound impact on an individual’s quality of life. The constant need to manage blood sugar levels, potential restrictions on dietary choices, and the fear of long-term complications can lead to feelings of frustration, isolation, and reduced quality of life.
Depression further compounds these challenges, amplifying feelings of sadness, anxiety, and hopelessness. Addressing the emotional impact of living with diabetes is vital to support individuals in maintaining a positive outlook and overall well-being.
Addressing Psychological Needs
Healthcare professionals should prioritize addressing the psychological needs of individuals living with Type 2 diabetes. By incorporating mental health assessments, offering counseling and psychoeducation, and implementing support programs, healthcare providers can help individuals cope with the psychological challenges associated with diabetes.
Understanding the unique experiences and concerns of individuals with comorbid depression and diabetes is essential for tailoring interventions and support. Additionally, addressing any stigma or self-blame associated with diabetes can contribute to improved mental health outcomes and overall quality of life.
Genetic Factors and Shared Vulnerabilities
Genetic factors play a significant role in both depression and Type 2 diabetes, with shared vulnerabilities contributing to their bidirectional relationship. Understanding the genetic underpinnings can help unravel the complex mechanisms behind these conditions.
Shared Genetic Variants
Recent research has identified shared genetic variants between depression and Type 2 diabetes. These genetic variants provide insight into the shared vulnerabilities and biological pathways underlying both conditions.
The study conducted by Dr. Cutler and his team at the Massachusetts General Hospital and Harvard Medical School identified seven genetic variants associated with both depression and diabetes. These findings highlight the importance of genetic susceptibility in the development of these conditions and suggest a shared genetic basis.
Role of Neurotransmitters and Hormones
Neurotransmitters and hormones play crucial roles in mood regulation and glucose metabolism, making them key players in the link between depression and Type 2 diabetes.
Abnormalities in neurotransmitters, such as serotonin, dopamine, and norepinephrine, have been implicated in both depression and diabetes. Dysregulation of these neurotransmitters can affect mood, energy levels, and cognitive function, as well as insulin sensitivity and glucose metabolism.
Hormones, including cortisol and insulin, also interact with neurotransmitter systems and have been implicated in both conditions. The dysregulation of these hormones can contribute to the development of insulin resistance and metabolic dysfunction, ultimately increasing the risk of diabetes and depressive symptoms.
Stress Response and Genetic Susceptibility
Stress response is intricately linked to both depression and Type 2 diabetes. Genetic susceptibility to stress and abnormalities in stress response systems can predispose individuals to develop both conditions.
The HPA axis, which regulates the body’s response to stress, is dysregulated in individuals with depression and diabetes. Genetic variations in stress response genes can alter the body’s ability to adapt to stressors, contributing to the development of both conditions.
Understanding the interplay between genetic vulnerabilities and stress response systems can help identify individuals at risk and inform targeted interventions for prevention and treatment.
Epigenetic Mechanisms
Epigenetics, the study of changes in gene expression that do not involve alterations in the DNA sequence, plays a significant role in the link between depression and Type 2 diabetes. Epigenetic modifications can be influenced by various environmental factors, including stress, diet, and lifestyle choices.
Epigenetic changes can affect the expression of genes involved in both depression and diabetes, influencing individual susceptibility to these conditions. Identifying specific epigenetic modifications associated with both conditions can provide valuable insights into their shared etiology and potential targets for intervention.
Intervention Strategies
Interventions for individuals with comorbid depression and Type 2 diabetes should adopt a comprehensive and multidisciplinary approach. A combination of psychotherapy, pharmacotherapy, integrated care models, and support groups can effectively address the complex needs of individuals dealing with both conditions.
Psychotherapy and Cognitive Behavioral Therapy
Psychotherapy, particularly cognitive-behavioral therapy (CBT), is an evidence-based treatment approach for both depression and diabetes. CBT focuses on identifying and modifying negative thought patterns and behaviors, promoting healthier coping strategies and self-care practices.
CBT can help individuals develop effective problem-solving skills, enhance emotional regulation, and improve adherence to diabetes self-care regimens. By addressing both psychological and behavioral factors, psychotherapy can contribute to better mental health outcomes and diabetes management.
Pharmacotherapy for Depression and Diabetes
Pharmacotherapy is an essential component of treatment for individuals with comorbid depression and diabetes. Antidepressant medications and glucose-lowering medications can be prescribed based on the severity of depressive symptoms and glycemic control.
Healthcare professionals should carefully consider the potential interactions between antidepressant medications and glucose-lowering medications, as certain antidepressants can affect glycemic control. Collaborative decision-making between mental health professionals and diabetes specialists can optimize medication management and minimize adverse effects.
Integrated Care Models
Integrated care models, involving close collaboration between primary care providers, mental health professionals, and diabetes specialists, are crucial for individuals with comorbid depression and Type 2 diabetes. These models facilitate coordinated care and ensure that individuals receive holistic and comprehensive support.
Integrated care models typically involve regular communication among healthcare providers, shared decision-making, and the implementation of evidence-based interventions. This collaborative approach optimizes treatment outcomes, improves the detection and management of both conditions, and enhances overall quality of care.
Support Groups and Peer Counseling
Support groups and peer counseling provide valuable social and emotional support for individuals with comorbid depression and Type 2 diabetes. Engaging with others who share similar experiences can reduce feelings of isolation, increase self-efficacy, and promote self-care behaviors.
Support groups can offer a safe space for individuals to share their challenges and triumphs, exchange information, and learn from one another. Peer counseling programs, where individuals with lived experiences provide support and guidance, can also play a vital role in fostering resilience and psychosocial well-being.
Public Health Implications
Considering the high prevalence of both depression and Type 2 diabetes, public health efforts should focus on raising awareness, addressing social determinants of health, incorporating mental health in diabetic clinics, and implementing early intervention and prevention programs.
Awareness Campaigns to Reduce Stigma
Awareness campaigns targeting the general population can help reduce stigma surrounding both depression and diabetes. By increasing public understanding and empathy, these campaigns can encourage individuals to seek help, promote early intervention, and reduce the burden of living with these conditions.
Addressing stigma is crucial in facilitating open conversations about mental health, encouraging help-seeking behaviors, and promoting a supportive environment for individuals with depression and Type 2 diabetes.
Addressing Social Determinants of Health
Social determinants of health, such as socioeconomic status, access to healthcare, and education, significantly impact both the prevalence and management of depression and diabetes. Public health efforts should focus on addressing these determinants to reduce health disparities and improve outcomes for all individuals.
By promoting equitable access to healthcare, providing resources for education and self-management, and addressing social and economic inequalities, public health initiatives can make significant strides in preventing and managing both conditions.
Incorporating Mental Health in Diabetic Clinics
Incorporating mental health services into diabetic clinics can improve the identification and management of depression in individuals with diabetes. By providing on-site mental health professionals or collaborating with community mental health organizations, healthcare providers can ensure that the mental health needs of individuals with diabetes are adequately addressed.
Routine mental health assessments, counseling, and psychoeducation can be seamlessly integrated into diabetes care, enhancing patient outcomes and overall well-being.
Early Intervention and Prevention Programs
Early intervention and prevention programs are essential in reducing the burden of both depression and Type 2 diabetes. Prevention efforts should emphasize the importance of identifying symptoms of depression early on and initiating appropriate interventions and support.
By focusing on preventing the development of Type 2 diabetes at the onset of depressive symptoms, healthcare professionals can foster better mental health outcomes and reduce the risk of diabetes-related complications.
Conclusion
The link between depression and Type 2 diabetes is multifaceted and bidirectional. Depression can play a direct role in the development of diabetes, while individuals with diabetes are at an increased risk of developing depression. Shared biological pathways, chronic stress, inflammation, genetic factors, and medication side effects contribute to this complex association.
Understanding and addressing the relationship between depression and Type 2 diabetes is crucial for optimizing patient care. Healthcare professionals should adopt a comprehensive and multidisciplinary approach, encompassing screening for depression, integrated care models, promoting physical activity and healthy lifestyle choices, and supporting emotional well-being.
Recognizing the bidirectional nature of this association and implementing a holistic approach to care can lead to improved outcomes for individuals dealing with both depression and Type 2 diabetes. Collaboration between healthcare professionals, awareness campaigns, and addressing social determinants of health are essential in reducing the burden of these conditions and fostering better mental and physical well-being.

LIV PURE REVIEW: THE NO.1 WEIGHT LOSS & LIVER CLEANSER SUPPLEMENT IN THE WORLD